Understanding Lupus: What It Is, Symptoms, and How to Manage It (Friendly Guide)
Lupus. You’ve probably heard the word before, but what is it really? For some, it’s just a mysterious disease mentioned in health articles or movies. For others, it’s a daily reality that affects their energy, joints, skin, and even internal organs.
In this guide, we’ll take a friendly, relaxed deep dive into lupus. We’ll explain what it is, its symptoms, how doctors diagnose it, treatments, lifestyle tips, and strategies for managing it without overwhelming medical jargon.
Whether you’re newly diagnosed, supporting a friend, or just curious, this guide will help you understand lupus in a clear, approachable way.
- What Is Lupus?
Lupus is an autoimmune disease. That means the body’s immune system, which usually fights off viruses and bacteria, mistakenly attacks healthy tissues.
Lupus can affect:
- Skin
- Joints
- Kidneys
- Heart
- Lungs
- Brain
- Blood cells
It’s a chronic disease, which means it lasts for a long time, often with periods of flare-ups (when symptoms get worse) and remissions (when symptoms improve).
There are different types of lupus:
- Systemic Lupus Erythematosus (SLE)
The most common type. It affects multiple organs and can vary from mild to severe.
- Cutaneous Lupus
Primarily affects the skin, causing rashes or lesions.
- Drug-Induced Lupus
Triggered by certain medications, usually reversible when the drug is stopped.
- Neonatal Lupus
Rare condition affecting newborns, caused by antibodies from the mother.
- How Common Is Lupus?
Lupus is relatively rare but more common than many people think. Some key facts:
- Around 5 million people worldwide have some form of lupus.
- Women are 9 times more likely to develop lupus than men.
- Most diagnoses occur between ages 15–45.
- Lupus is more common in people of African, Asian, Hispanic, and Native American descent.
- What Causes Lupus?
The exact cause isn’t fully understood. Experts believe it’s a combination of genetic, environmental, and hormonal factors.
- Genetics
Having a family member with lupus increases your risk, but it’s not guaranteed.
- Hormones
Estrogen may play a role since lupus affects more women than men.
- Environmental Triggers
- Sunlight (UV exposure)
- Infections
- Stress
- Certain medications
- Immune System Dysfunction
The immune system loses its ability to distinguish between healthy tissue and harmful invaders.
- Common Symptoms of Lupus
Lupus is called “the great imitator” because symptoms often mimic other conditions. They can also come and go, making diagnosis tricky.
Some common signs include:
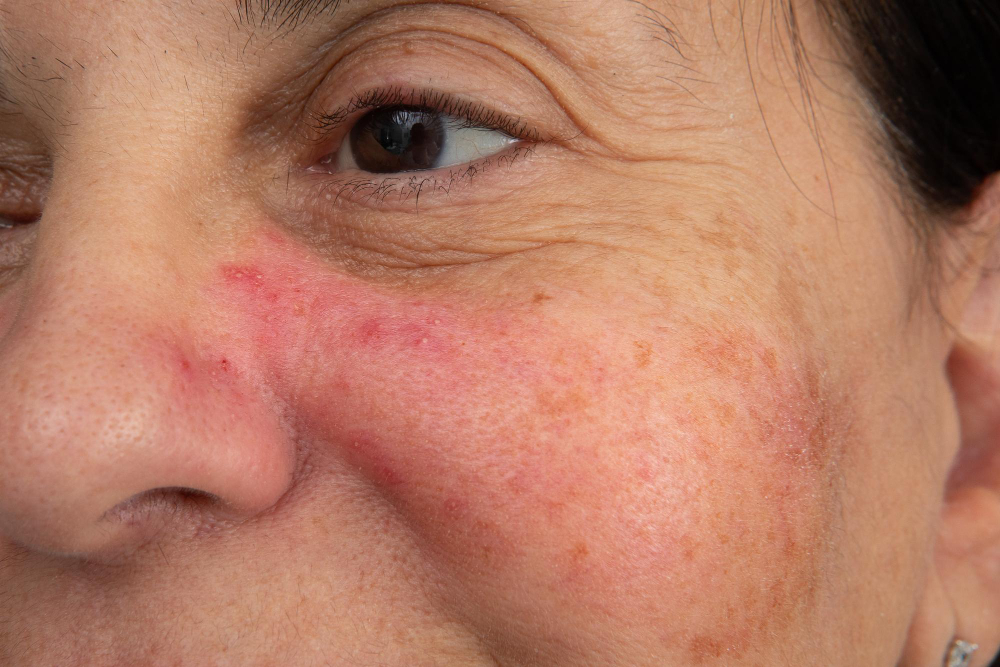
Skin Symptoms
- Butterfly-shaped rash across cheeks and nose
- Red or purple rashes on other body parts
- Sun sensitivity (photosensitivity)
- Hair loss
Joint Symptoms
- Pain, stiffness, swelling (often hands, wrists, knees)
- Arthritis-like symptoms
Fatigue
- Extreme tiredness not relieved by sleep
- Low energy levels
Fever
- Low-grade fever during flare-ups
Organ-Specific Symptoms
- Kidney problems: swelling, changes in urination
- Heart issues: chest pain, inflammation
- Lung problems: shortness of breath, pleuritis
- Brain: confusion, headaches, memory issues
Other Symptoms
- Anemia or low blood cell counts
- Mouth or nose ulcers
- Raynaud’s phenomenon (fingers/toes turn white or blue in cold)
- How Lupus Is Diagnosed
Diagnosing lupus can be challenging because symptoms overlap with other diseases. Doctors use a combination of:
- Medical History
Detailed questions about symptoms, family history, and flare patterns.
- Physical Examination
Looking for rashes, joint swelling, or other visible signs.
- Blood Tests
- ANA (Antinuclear Antibody) test: positive in most lupus patients
- Anti-dsDNA, anti-Smith antibodies
- Complete blood count (CBC)
- Kidney and liver function tests
- Urine Tests
Detect kidney involvement, protein, or blood in urine.
- Imaging Tests
X-rays or ultrasounds may be used to check joints or organs.
- Lupus Flares: What They Are and How to Spot Them
A flare is when lupus symptoms suddenly get worse. Triggers include:
- Stress
- Sun exposure
- Infections
- Hormonal changes
- Certain medications
Signs of a flare:
- Increased fatigue
- Joint pain or swelling
- Fever
- Rashes or lesions
- Changes in kidney function
Tip: Keeping a symptom diary helps you notice patterns and triggers.
- Treatment Options for Lupus
There’s no universal cure, but treatments focus on managing symptoms, preventing flares, and protecting organs.
- Medications
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs)
- Reduce pain, swelling, and fever
- Example: ibuprofen
- Corticosteroids
- Powerful anti-inflammatory
- Often used during flares
- Must be monitored due to side effects
- Antimalarials
- Hydroxychloroquine (Plaquenil) reduces flares, especially skin and joint issues
- Immunosuppressants
- Methotrexate, azathioprine, or mycophenolate
- Used for severe organ involvement
- Biologics
- Target specific immune pathways
- Example: Belimumab (Benlysta)
- Lifestyle Tips to Manage Lupus
Medical treatment is crucial, but lifestyle changes also help improve quality of life.
- Protect Yourself from the Sun
- Wear sunscreen SPF 30+
- Use hats and long sleeves
- Avoid peak sunlight hours
- Balanced Diet
- Anti-inflammatory foods: fruits, vegetables, fatty fish, whole grains
- Limit processed foods, sugar, and trans fats
- Stay hydrated
- Regular, Gentle Exercise
- Low-impact exercises: walking, swimming, yoga
- Helps joints, muscles, and mood
- Stress Management
- Meditation, deep breathing, journaling
- Avoid triggers when possible
- Sleep
- Prioritize 7–9 hours nightly
- Helps immune system and energy
- Avoid Smoking & Limit Alcohol
- Smoking worsens lupus complications
- Alcohol may interact with medications
- Regular Checkups
- Monitor kidney function, blood pressure, and labs regularly
- Coping With Lupus Emotionally
Living with a chronic disease is challenging. Emotional health matters as much as physical health.
- Join support groups (online or local)
- Talk to friends or family
- Consider counseling or therapy
- Practice mindfulness and relaxation techniques
- Pregnancy and Lupus
Pregnancy is possible but requires careful planning:
- Consult a rheumatologist before conception
- Lupus flares can occur during pregnancy
- Some medications may need adjustment
- Frequent monitoring ensures maternal and fetal safety
- Myths and Misconceptions About Lupus
Myth 1: Lupus is contagious
Truth: Lupus is autoimmune, not infectious.
Myth 2: Only women get lupus
Truth: Women are more common, but men can have it too.
Myth 3: Lupus always looks severe
Truth: Symptoms vary — some people have mild disease for years.
Myth 4: You can’t live a normal life
Truth: With treatment, many people lead full, active lives.
- When to See a Doctor
Seek medical attention if you notice:
- Persistent fatigue or fever
- Joint swelling or pain
- New rashes, especially butterfly-shaped
- Shortness of breath or chest pain
- Changes in urination
- Confusion or severe headaches
Early intervention prevents complications.
- Lupus and Other Health Conditions
Lupus can increase the risk of:
- Kidney disease (lupus nephritis)
- Cardiovascular disease
- Osteoporosis (especially with steroid use)
- Infections (due to immune system or medications)
- Blood clots (antiphospholipid syndrome)
Regular checkups and lifestyle choices reduce these risks.
- Complementary Approaches
Some people use complementary methods alongside medical treatment:
- Yoga and tai chi for flexibility and stress
- Meditation or mindfulness
- Acupuncture for pain management
- Omega-3 supplements (with doctor approval)
Always check with your doctor before trying new supplements or therapies.
- Supporting Someone With Lupus
If a loved one has lupus:
- Educate yourself about the disease
- Be patient and understanding
- Offer practical support (meals, transportation)
- Encourage rest and self-care
- Listen without judgment
Emotional support is just as important as medical care.
- Lupus Research and Hope for the Future
Research is ongoing. New treatments, biologics, and better diagnostic tools are improving outcomes.
Some exciting areas include:
- Personalized medicine
- Targeted immune therapies
- Safer steroid alternatives
- Better flare prediction and prevention
Hope and progress are real. Living with lupus is challenging, but medical science is advancing.
- Summary: Key Takeaways
- Lupus is an autoimmune disease that can affect multiple organs.
- Symptoms vary widely and often come in flares.
- Early diagnosis and treatment prevent complications.
- Medications and lifestyle changes work together for management.
- Protect yourself from the sun, eat well, exercise gently, and manage stress.
- Emotional support and counseling matter.
- Research is advancing, offering hope for better treatments.
- Final Thoughts
Lupus may be unpredictable, but knowledge and support make a huge difference.
Living with lupus isn’t easy, but it doesn’t define you. With the right treatment plan, healthy habits, and emotional support, people with lupus can live full, active, meaningful lives.
Take control where you can, be gentle with yourself, and trust the journey — you’re not alone.




